Intrathecal Route: Mechanism, Uses, and Challenges
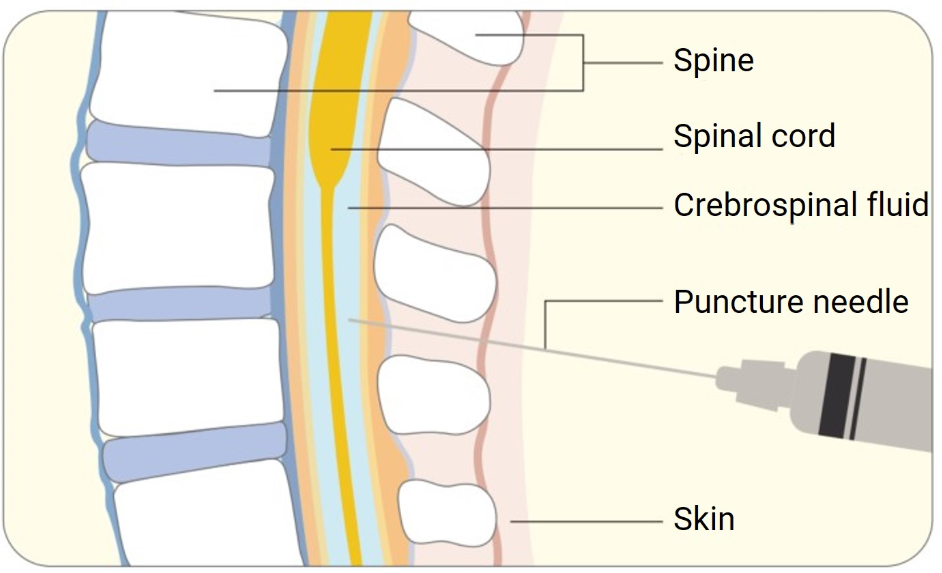
The intrathecal route definition refers to a targeted method of delivering drugs directly into the cerebrospinal fluid (CSF), allowing for localization of treatment to the central nervous system (CNS). This route bypasses the blood-brain barrier, offering enhanced therapeutic effects for patients with neurological conditions, certain cancers, and chronic pain. Due to its direct access to the CNS, intrathecal drug delivery can achieve desired pharmacological responses with reduced systemic exposure and toxicity. Despite its potential, the method demands precise technique and rigorous safety standards. Understanding how the intrathecal route works, its applications, and the challenges it presents is crucial for advancing CNS-targeted therapies and improving patient outcomes. This blog explores the mechanism, uses, and challenges associated with intrathecal administration.
How the Intrathecal Route Works in Drug Delivery
Mechanism of Intrathecal Administration and CSF Dynamics
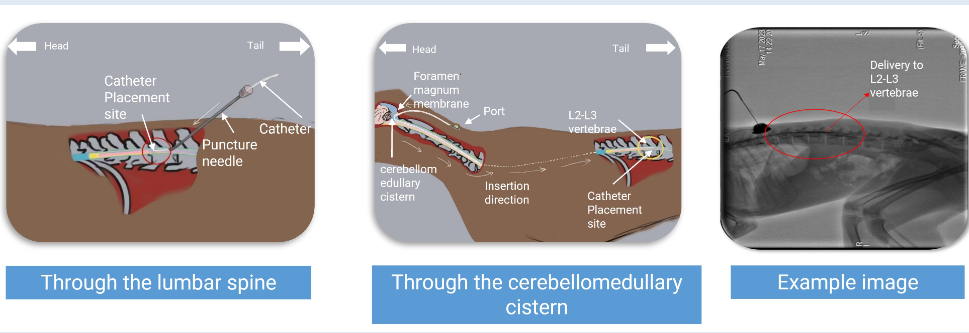
Intrathecal administration involves injecting medication into the CSF, typically via lumbar puncture in the lower spine. This method ensures direct contact with the CNS, as opposed to systemic routes that require traversing the blood-brain barrier. Once injected, the drug diffuses through the CSF, distributing along the spinal canal and brain ventricles. The dynamics of CSF flow, influenced by factors like posture and respiratory activity, affect the distribution and dilution of the drug. This targeted delivery ensures that the medication reaches the intended receptors rapidly, enhancing efficacy while minimizing peripheral exposure. The precise technique involved necessitates trained professionals to mitigate risks such as infection or nerve damage during administration.
Pharmacokinetics and Drug Distribution After Intrathecal Dosing
After intrathecal dosing, drugs encounter unique pharmacokinetic properties distinct from systemic administration. The concentration gradient between the CSF and surrounding tissues drives diffusion, allowing for rapid localized action. However, this approach also poses challenges in maintaining consistent drug levels due to CSF turnover, where the fluid is replaced several times a day. Understanding these dynamics is crucial for dosing regimens to ensure therapeutic effectiveness while avoiding toxicity. Drug molecules require specific physicochemical properties, such as solubility and stability, to sustain therapeutic concentrations within the CSF. Researchers are continually refining models to predict and optimize drug behavior in this equilibrated environment, ensuring precise dosing protocols tailored to patient needs.
Clinical and Research Applications of the Intrathecal Route
Therapeutic Uses in Pain, Oncology, and Neurological Diseases
The intrathecal route is pivotal in treating severe pain, particularly when systemic opioids are ineffective or pose high risk. Controlled doses of analgesics directly target pain pathways, providing substantial relief. Oncology applications include chemotherapeutic agents for cancers that have metastasized to the CNS, offering targeted action with reduced systemic impact. Furthermore, for neurological diseases like spasticity in multiple sclerosis or chronic neurodegenerative conditions, intrathecal therapy delivers medications that modulate nerve activity, improving quality of life. The precision of intrathecal delivery makes it indispensable for conditions requiring high CNS drug concentrations, translating to enhanced patient outcomes and reduced side effects.
Role of Intrathecal Delivery in CNS Drug Development Services
Intrathecal delivery is increasingly vital in CNS drug development. By bypassing the blood-brain barrier, it facilitates novel therapeutic options for diseases like Alzheimer’s and Parkinson’s. Research focuses on optimizing molecular designs of drugs to leverage the intrathecal pathway. This route enables high-concentration administration crucial for effective CNS treatments, accelerating developments in biologics and gene therapies. Companies specializing in CNS therapeutics are advancing intrathecal formulations to enhance drug efficacy, minimize systemic exposure, and support personalized medicine initiatives. Collaboration with regulatory bodies ensures safety and compliance, fostering innovation in CNS-targeted treatments and making significant strides in addressing unmet medical needs.
Key Challenges and Considerations of Intrathecal Administration
Safety Risks, Technical Barriers, and Regulatory Concerns
Intrathecal administration presents safety risks such as infection risk, accidental injury to nerves, and potential toxicity. Precise administration techniques are essential, requiring skilled personnel to navigate these challenges reliably. Technical barriers include difficulties in maintaining consistent drug delivery and monitoring effects. Regulatory concerns arise around ensuring the safety and efficacy of intrathecal drugs, demanding rigorous trials and post-approval surveillance. These complexities necessitate comprehensive protocols and robust training programs. To mitigate risks, developers must adhere to stringent regulatory guidance and improve patient monitoring technologies, ensuring that the benefits of intrathecal delivery outweigh potential adverse effects.
See also: Lifestyle Choices and Their Impact on Long-Term Health
Translational Challenges and Study Design in Preclinical Models
Translating intrathecal drug delivery from preclinical models to human applications involves overcoming significant hurdles. Preclinical studies must accurately mimic human CSF dynamics and neuroarchitecture to predict clinical outcomes reliably. Designing studies that address interspecies differences in CSF production, flow, and volume is crucial. Challenges include optimizing drug formulations for intrathecal stability and bioavailability. Researchers face difficulties in consistent dosing and achieving comparable pharmacokinetics across models. Collaboration between multidisciplinary teams aids in refining animal models and study designs to better forecast human responses, ensuring translational success and advancement in intrathecal therapeutic interventions.
Conclusion
The intrathecal route presents promising avenues for targeted CNS therapies, offering substantial benefits in pain management, oncology, and neurological conditions. By bypassing systemic barriers, it provides direct access to the CNS, driving advancements in drug development and personalized medicine. However, the administration demands precise technical skills and adherence to rigorous safety standards to overcome associated risks and challenges. Continued research and collaboration are vital for optimizing drug formulations and administration techniques, ensuring effective and safe outcomes for patients. As innovation progresses, intrathecal delivery is poised to play a crucial role in addressing complex CNS disorders.